Age-Related Macular Degeneration

Age-related macular degeneration (AMD) is one of the most common causes of poor vision after age 60, affecting approximately 30% of people over the age of 75. AMD is a deterioration or breakdown of the macula. The macula is a small area at the center of the retina that allows us to see fine details and perform activities such as reading, driving, and recognizing faces.
The visual symptoms of AMD involve loss of central vision and visual distortion; peripheral (side) vision is usually not affected. Thus most individuals with AMD can continue to perform most activities, even with advanced disease.
There have been major recent breakthroughs in understanding the causes of AMD. Heredity is very important, and may account for as many as 70% of all cases. Scientists have recently identified several genes that increase the risk for developing AMD. In the near future, genetic screening will be available to identify those individuals at highest risk. Age is a very important risk factor; others include smoking, obesity, and cardiovascular disease. Men and dark-skinned races have a lower risk.
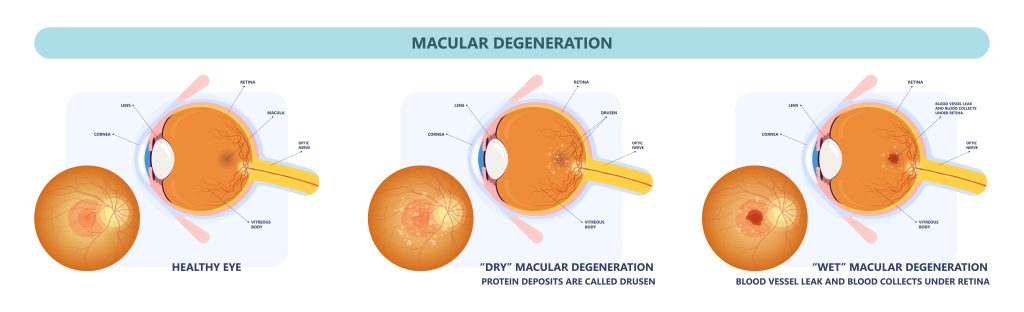
Eighty five percent of people with AMD have atrophic or “dry” AMD, which results in thinning and deposition of abnormal deposits beneath the macula (drusen). Dry AMD takes many years to develop. An over-the-counter vitamin regimen (the AREDS formula) has been shown to slow progression of dry AMD in some cases, and your doctor may recommend this for you. A specific form of dry AMD called geographic atrophy can result in severe visual loss; most patients with the dry form, however, suffer mild to moderate visual loss, and many patients are asymptomatic.
Exudative or “wet” AMD is less common (occurring in fifteen percent of people with AMD) but is more serious. In the wet form, abnormal blood vessels (choroidal neovascularization) grow beneath the retina, allowing leakage of fluid and blood and creating distortion or a blind spot in the center of vision. If the blood vessels are not growing directly beneath the center of the macula (the fovea), laser surgery is sometimes effective. This procedure usually does not improve vision but prevents further loss of vision.
Unfortunately, in most cases, blood vessel growth occurs directly beneath the fovea. For such cases, since late 2005 we have been using pharmacological agents that block the leakage from these abnormal blood vessels. These medications are injected directly into the eye in a painless, simple office procedure, and have revolutionized AMD treatment. In several studies, treatment has been found to maintain vision in 95% of patients for an indefinite time period; 40% of patients maintain a vision of 20/40 or better, good enough for an unlimited driver’s license. At Eye Care of Maine, we have hundreds of patients under Anti-VEGF (also known as anti-vascular endothelial growth factor) treatment, depending on various circumstances.
The main drawback of Anti-VEGF treatment is the need for frequent follow-up visits, and the need for frequent injections. Most of our wet AMD patients are seen every four to six weeks, however many are able to go 2-3 months between treatments. Click here for more information about Anti-VEGF treatments.
Promising AMD research is being done on many fronts. Unfortunately, despite our best efforts, some patients will end up losing vision. For these patients, low vision aids such as high-intensity reading lamps and various types of magnifying aids are very helpful in assisting people with AMD to make the most of their remaining vision.
